Introducing Integrity AI
Empower your payment integrity team with proactive, AI-driven solutions—catching overpayments in-house, saving time and cutting vendor fees.
80%
25%
$24M
Up to 80% of healthcare overpayments arise from recurring patterns—recovering them in-house can significantly reduce third-party fees.
External PI vendors may charge more than 25% of recovered amounts, causing major revenue leakage.
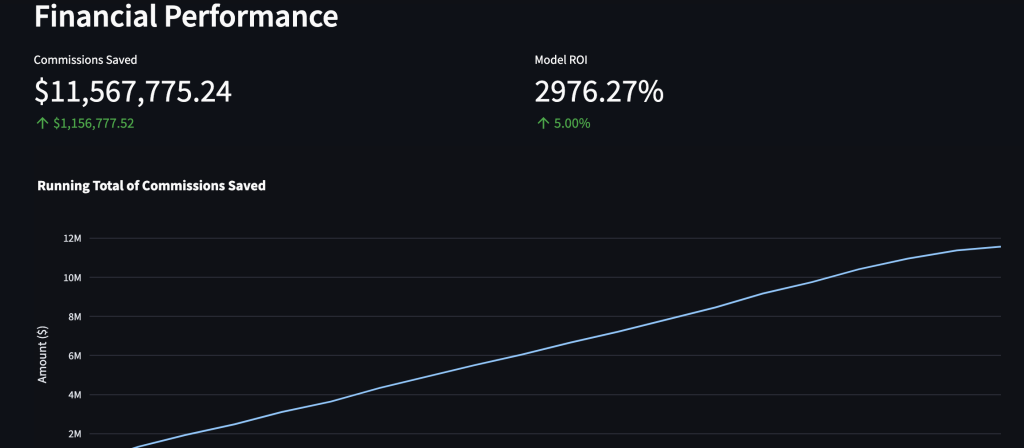
A midsized health plan could cut up to $24 million annually in vendor commissions by equipping an internal team with our advanced ML solution.
IntegrityAI Model
Our AI/ML Stack
Our AI/ML stack is built on three key layers—each designed to streamline claim analysis, identify repeatable overpayments, and continually refine outcomes. By leveraging these layers, you can cut vendor fees and boost payment accuracy across your healthcare programs.
Program Optimization
Leverages feedback loops and real-time analytics to fine-tune detection rules, ensuring consistent improvement in results. Each iteration of your program becomes increasingly precise and resource-efficient.
Autonomous Task Execution
ML-driven modules independently manage repeatable, high-volume claim assessments—dramatically cutting manual intervention and improving turnaround times. This automation allows your team to focus on higher-level strategic tasks.
Foundational Models
Core AI algorithms trained on vast amounts of claims data and policies—forming the backbone of accurate, data-driven insights. These models learn continuously, adapting to new patterns and emerging industry shifts.
Featured Article
Why AI is the Perfect Neutral Arbiter for Health Care Claims
There are three “levels” of AI you can test a product for, specifically in the context of claims processing. Asking the right questions not only helps you determine what level of AI a product uses, but also whether it truly relies on AI at all. Discover how these “levels” drive more accurate and objective claim evaluations.